US Healthcare is a Burning Platform and Doctors are Jumping
HDai Point of View
Native-AI Healthcare: A New Super-Category to Fix Outpatient Medicine
Outpatient healthcare in the US is a $1 trillion mess. Americans spend twice as much as peer nations—yet suffer worse outcomes. Primary care patients in community health centers suffer heart failure and go blind because they lack access to specialty care. Squeezed between payor fee caps and rising operating costs- physician income is being crushed. Economic pressures compounded by excessive administrative demands have caused widespread burnout in the healthcare workforce and a record number of physicians and other skilled healthcare workers to quit medicine.
The AI-Revolution is Poised to Disrupt Industries
As the next tsunami of digital technology, there is widespread consensus that AI will reshape entire industries, unlocking value and creating entirely novel models of service and productivity. From digital customer service agents to self-driving cars; from automating legal workflows to robotic surgery. Yet, no clear roadmap exists for how - or if - this revolutionary technology can be harnessed to fix healthcare’s imminent collapse.
Beyond AI Point Solutions—A Native-AI Platform to Reengineer the Clinical Encounter
Harvey for Healthcare
And it’s Working
Native-AI Healthcare is a $0B Market — Today
An All-New Tech Stack to Re-Engineer Healthcare’s Value-Generating Transaction
How Native AI Healthcare Will Fix Our Broken System
Creating a Category Choice for Healthcare Providers
Cost. Automation of tasks by AI will dramatically reduce the practices’ labor costs to provide care. Primary care patients access to specialty care will help keep diseases under control and reduce the costly use of emergency rooms and urgent care clinics.
Access. Virtual encounters on the Platform will make many outpatient services boundary-less. Specialty care will become available in primary care settings and primary care can be extended to rural health centers and school clinics.
Quality. The Platform’s use of multi-modal and generative AI will revolutionize disease detection and precision medicine solutions. Patients will experience a modern, differentiated encounter and become more engaged in their care. Over time, Native AI-Encounters will become the new standard of care.
Provider Income & Workforce Satisfaction.
Later versions of the Native-AI encounter platforms will feature proprietary products and services that will be self-pay, premium priced, and not subject to payor fee caps. This model will end the commoditization of physician services and free providers from the economic tyranny imposed by payors’ consignment contracts. Native-AI healthcare will usher in a new era of sustainable practice economics—supporting a happier, more autonomous, and sustainable clinical workforce.
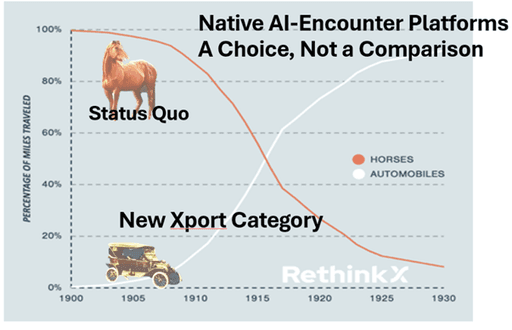
The introduction of the motorcar over a century ago forced consumers to make a choice: Stay with obsolete horse-driven carriages or embrace an emerging Super-Category of transportation vehicles powered by the internal combustion engine.
As Native-AI Healthcare becomes available across outpatient specialties, providers will face a similar choice: stay on a legacy platform destined for collapse or embrace the new Super-Category of Native-AI healthcare that resolves medicine’s unsustainable problems of cost, quality, access, and falling provider income.
Unlike most AI-health startups building narrow point solutions—scribes, chatbots, and coders—HDai is rebuilding the core value-creating transaction itself: the clinical encounter. AI tools may improve individual steps, but they cannot fix a broken system. Just as Harvey didn’t automate spellcheck for law, HDai isn’t auto-scribing. We’re re-architecting the entire encounter stack with the latest digital diagnostics, intelligent agents, multimodal models, and automation. This is a platform-level solution that will absorb point tools, not compete with them.
In law, Harvey proved that vertical AI platforms can transform legacy professional workflows and generate massive enterprise value. In May 2025, Harvey AI’s valuation soared to $5 billion, proving that vertical AI platforms in professional services led by domain experts can reengineer the core value-creating transaction in their industry.
HDai is bringing that same playbook to healthcare—a far larger, more fragmented, and dysfunctional industry—where the core transaction, the doctor-patient encounter, is broken, obsolete, and the root cause of healthcare’s unsolved ailments.
Just as Harvey is becoming the category-defining platform for Legal AI, HDai is positioned to define Native-AI Healthcare by rebuilding the encounter start to finish using intelligent agents, multimodal diagnostics, and automation. This reinvention will unlock scalable solutions to healthcare’s intractable problems of cost, access, quality, and plummeting physician income.
Just as Harvey redefined legal workflows to create a multibillion-dollar category in law, HDai is building the first scalable platform for Native-AI healthcare delivery — one that doesn’t just optimize the existing system, but replaces it. We’re not competing for share in an existing market; we’re creating a new Super-Category of healthcare that can be scaled across multiple outpatient specialties as outlined in the Category Architecture Table.
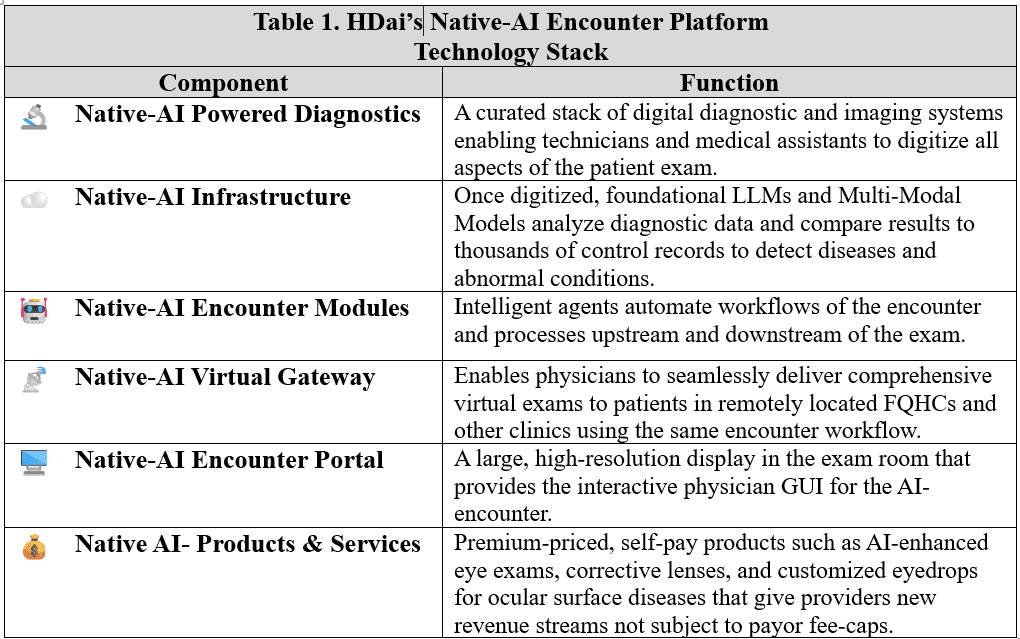
HDai's Native-AI Encounter Platform is a new technology stack that brings the power of AI to where the work gets done in outpatient medicine – the outpatient encounter. The existing categories of medical diagnostics, EMR, and telehealth platforms were built to serve and sustain the conventional doctor-patient encounter. They are incapable of fixing healthcare’s burning platform.
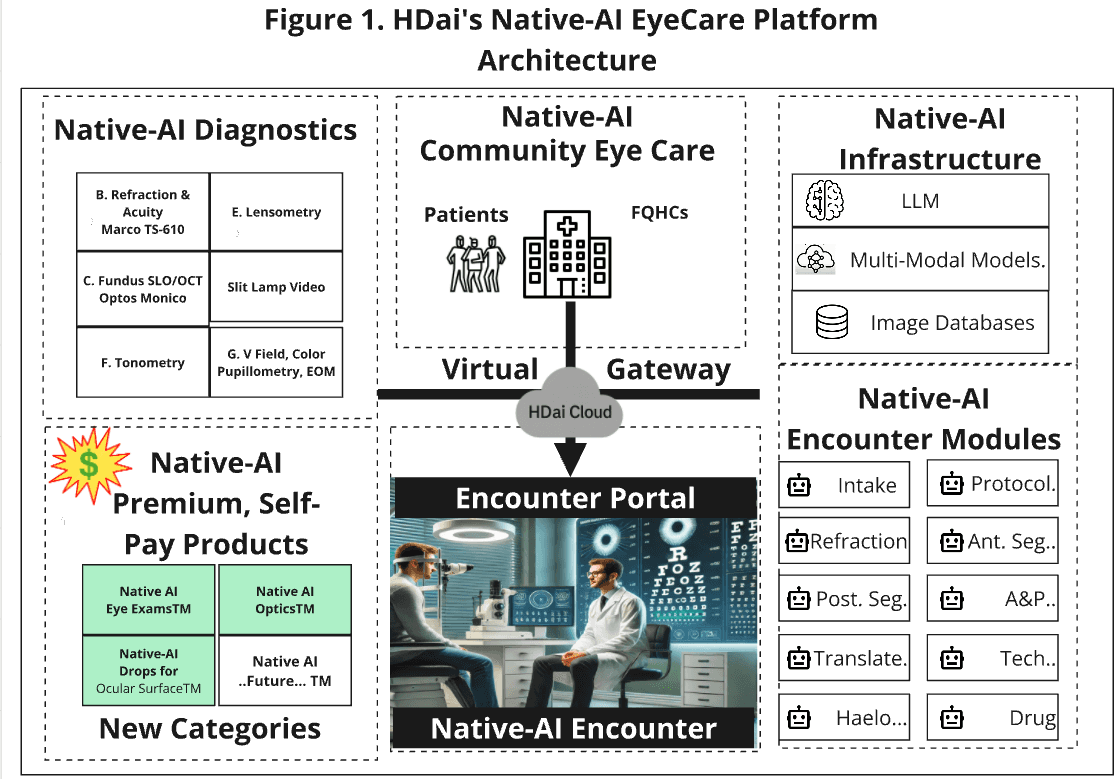
The HDai Native-AI Encounter Platform is built on a novel technology stack designed to bring artificial intelligence into the core workflows of outpatient care. Figure 1 illustrates the platform’s key components, with corresponding functions detailed in the table below. Each module is engineered for rapid deployment: it either requires no regulatory approval, qualifies under the FDA’s Clinical Decision Support (CDS) safe harbor, or is eligible for 510(k) clearance—allowing HDai to scale quickly while maintaining compliance.
These are not projections. They are in-market results from real customers, real patients, real doctors, and real revenue. They confirm that HDai has achieved category-market fit built around a physician-empowering platform.
HDai’s first deployment is a market entry wedge into the FQHC market to deliver comprehensive virtual eye exams to underserved patients — creating a new category of Native-AI Community Eye Care. And the results are unprecedented:
• Unit-level profitability from day one
• 60% gross margins, expandable to 93% at scale
• LTV:CAC > 15:1, placing us in the top tier of venture-scale efficiency
• 30% month-over-month growth, with accelerating demand
• Net Promoter Score = 100 from the first 75 paying patients —unheard of in healthcare
• Category validation: 30:1 patient preference for the new Native-AI virtual exam
• Partner FQHCs: New revenue w/30-40% margins and eye care for their at-risk patients
Facing a doctor shortage worsened by a hemorrhage of its frontline workforce, the US healthcare system is on an unsustainable path. Urgent solutions are needed to the unsolved problems of costs, access, quality, and plummeting practice income.